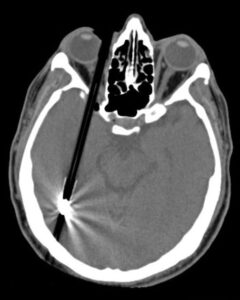
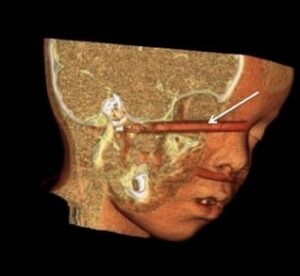
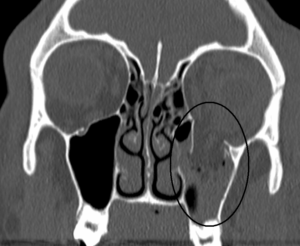
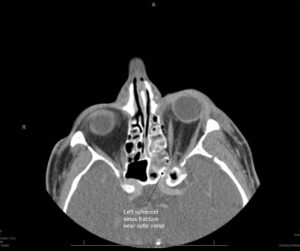
The bony, pear-shaped socket that surrounds and protects the eye is called the orbit. When an object larger than the size of the orbital entrance hits the eye but doesn’t penetrate, the force can literally cause a “blow out” of part of the orbit. The bone that forms the floor of the orbit is particularly prone to this type of fracture, known as a blow-out fracture. Blow-out fractures often occur when a fist or ball, or the dashboard of a car during a motor vehicle accident, strikes the eye. Emergency Trauma services in Mumbai are available at Wavikar Eye Hospital.A possible complication of orbital floor fracture is that the eye may partially drop down into the maxillary sinus, which is directly beneath the orbital floor, trapping some of the muscles that move the eye.