![]() Medically Reviewed
Medically Reviewed
Symblepharon
Symblepharon is a condition where the inner eyelid sticks to the surface of the eye (conjunctiva) due to scarring. It is usually caused by injury, infection, or inflammation and can restrict eye movement or cause discomfort.
If your eyelid feels “stuck” to your eyeball, or you notice a web‑like tissue between the lid and the white of your eye, you may be dealing with symblepharon. This condition occurs when the inner eyelid and the eyeball’s surface become abnormally attached due to scarring from inflammation, infection, or injury.
Skilled ophthalmologists at Wavikar Eye Institute explain that symblepharon happens when severe inflammation causes the eye tissues to swell and stick together. After the inflammation subsides, scars can form, permanently fusing the conjunctival layers and creating one or more adhesions. Chronic or recurrent inflammation increases the risk of repeat episodes of symblepharon.
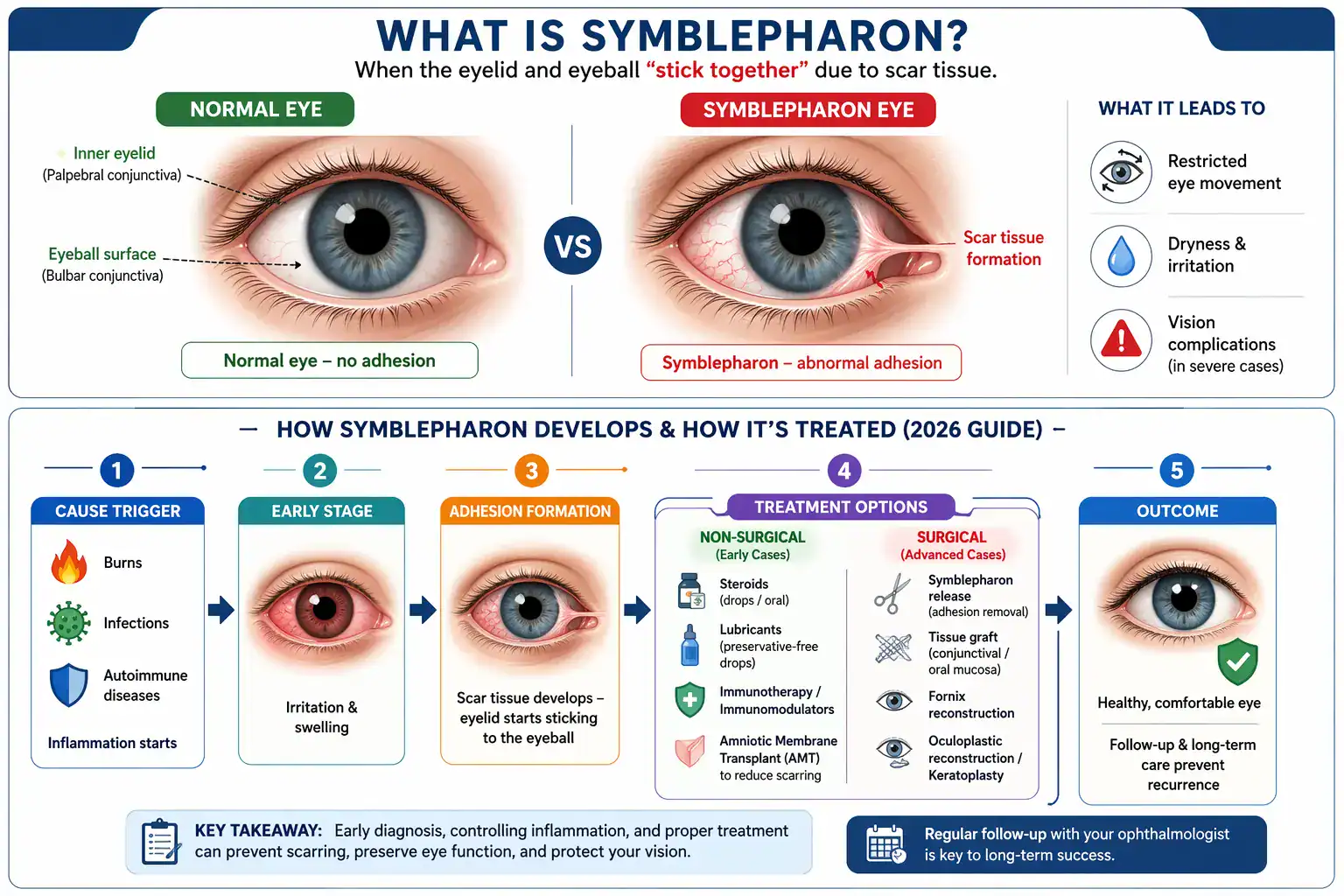
Medical treatment focuses on controlling the underlying cause and may include:
- Corticosteroids to reduce inflammation.
- Antibiotics or antivirals for bacterial or viral infections.
- Immunomodulators for autoimmune diseases affecting the ocular surface.
Explore this guide to know what symblepharon is, why it happens, early warning signs, and the most effective treatments in 2026.
A Quick Glance
Section | Key takeaway |
What it is | Abnormal adhesion between inner eyelid and eyeball. |
Main causes | Inflammation, infection, burns, trauma, surgery, autoimmune disease. |
Risk factors | Eye burns, severe conjunctivitis, autoimmune disease, dry eye, prior surgery. |
Why early treatment matters | Prevents permanent scarring, vision loss, and complex surgery. |
Types of symblepharon | Anterior, posterior, total, simple, cicatricial, fornix, congenital. |
Symptoms & complications | Web‑like band, limited movement, dry eye, redness, tearing, double vision. |
Diagnosis | Eye exam, slit‑lamp, and tests if needed. |
Medical treatment | Steroids, antibiotics/antivirals, immunomodulators, lubricants, amniotic membrane. |
Surgery options | Symblepharon release, grafts, fornix/oculoplastic reconstruction, corneal transplant. |
What Is Symblepharon? (Simple Definition)
Symblepharon is an abnormal adhesion between the palpebral conjunctiva (lining inside the eyelid) and the bulbar conjunctiva (covering the white of the eye).
It connects:
- Palpebral conjunctiva (inner eyelid)
- Bulbar conjunctiva (white of the eye)
Leads to:
- Restricted eye movement
- Dryness and irritation
- Vision complications (in severe cases)
In simple terms: The eyelid and eyeball “stick together” due to damage and healing with scar tissue.
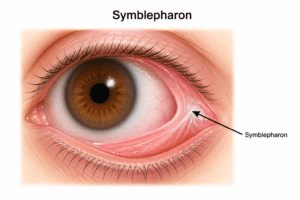
Why Does Symblepharon Happen? (Root Causes)
Symblepharon usually develops after severe or chronic inflammation, injury, or autoimmune disease affecting the ocular surface. Common triggers include infections, burns, surgeries, and systemic autoimmune conditions that scar the conjunctiva.
Top Causes in 2026
Cause category | Examples of conditions / triggers |
Infections & inflammation | Severe conjunctivitis, adenoviral keratoconjunctivitis, ocular herpes, trachoma. |
Eye injuries & burns | Chemical burns, thermal burns, ocular trauma, surgery complications. |
Autoimmune & systemic | Mucous membrane pemphigoid, Stevens‑Johnson syndrome, sarcoidosis, scleroderma, etc. |
Medication / reaction | Adverse drug reactions, graft‑versus‑host disease, chronic ocular surface inflammation. |
Who is at Higher Risk of Symblepharon?
Risk factors for developing symblepharon are:
Risk factor | Why it increases risk |
Chemical or thermal eye burns | Damage to conjunctiva and cornea promotes |
Severe untreated conjunctivitis | Chronic inflammation leads to fibrosis and |
Autoimmune mucous membrane disorders | Conditions like ocular cicatricial pemphigoid |
Previous ocular surgeries | Surgery‑related inflammation or complications can |
Chronic dry eye or ocular surface disease | Constant irritation and poor healing increase |
Stevens‑Johnson syndrome history | Severe mucocutaneous disease often leaves |
People Also Ask Two Common Questions
Is symblepharon curable?
Symblepharon can often be corrected with surgery and medical treatment, but long‑term control of the underlying disease is needed to prevent recurrence.
Is symblepharon painful?
Yes, it can cause discomfort or pain, especially with inflammation, restricted eye movement, or corneal involvement. Follow your doctor advice to alleviate the pain.
Why Early Treatment of Symblepharon Is Critical
Timing | Outcome |
Early treatment | Prevents scarring and preserves vision |
Delayed care | Leads to fornix loss, corneal damage, complex surgery |
Regular follow-up | Reduces recurrence risk |
Symblepharon may begin as mild conjunctival inflammation, but progressive scarring can permanently alter eye structure if left untreated. Early medical management can prevent adhesions from worsening and reduce the risk of corneal damage, restricted eye movement, and vision impairment. Prompt ophthalmic evaluation significantly improves long-term visual outcomes.
Risk Factors That Increase Symblepharon Development
Certain individuals are at higher risk of developing symblepharon:
- History of chemical or thermal eye burns
- Severe untreated conjunctivitis
- Autoimmune disorders affecting mucous membranes
- Previous ocular surgeries
- Chronic dry eye or ocular surface inflammation
- Stevens-Johnson Syndrome history
Patients with these risk factors should undergo regular ophthalmic monitoring to prevent progressive scarring.
Individuals with autoimmune or chronic inflammatory eye conditions should undergo periodic eye examinations to detect early conjunctival scarring before adhesions become permanent.
Are There Different Types of Symblepharon?
Variant | Description |
Anterior Symblepharon | Adhesion between the eyelid edge and the eyeball surface. |
Posterior Symblepharon | Involves the conjunctival fornix or cul-de-sac, leading to deeper adhesions. |
Total Symblepharon | Complete fusion of the eyelid to the globe, obliterating the fornix. |
Simple Symblepharon | Limited adhesions between the eyelid and eyeball conjunctiva, often affecting a small area. |
Cicatricial Symblepharon | Extensive adhesions resulting from significant inflammation and scarring of the conjunctiva. |
Fornix Symblepharon | Adhesions specifically form in the conjunctival fornices, the recesses between the eyeball and eyelids. |
Congenital Symblepharon | Rare form present at birth, sometimes associated with conditions like cryptophthalmos. |
What Symptoms Should You Watch For?
Symptom / sign | What it may indicate |
Visible band between eyelid and eye | Direct adhesion of conjunctiva; classic sign of |
Reduced eye movement | Adhesions pulling the globe; may cause diplopia |
Difficulty opening or closing eyelids | Ptosis, lagophthalmos, or entropion due to |
Chronic eye irritation, redness, tearing | Ocular surface inflammation and dryness. |
Light sensitivity and burning | Corneal exposure or epithelial damage. |
Noticeable dry eye or mucus stringiness | Tear‑film disruption due to fornix loss and |
Symblepharon is visible in your eye. It seems to be a strip of tissue that joins your eyeball and inner eyelid. If it is not visible to you directly, you may detect that your eyeball can no longer move in all of its previous ways or that your eyelid does not open completely. Other possible symblepharon complications include:
Ptosis: This condition pulls your eyelid down, resulting in eyelid drooping
Entropion: Inward pushing of eye balls
Lagophthalmos: Failure to close your eyes completely
Diplopia: Limited eyeball movement, resulting in double vision
Other symptoms include
Eye irritation
Redness
Tearing
Light sensitivity
Dry eye
How is Symblepharon Diagnosed?
With an eye exam, your eye care professional can detect symblepharon. To make eye examination simpler, they might give you eye drops. They will closely examine which tissues are linked and what is the site of attachment during your examination. Additionally, they will look for any complication related to your particular type of symblepharon.
In the event that your doctor is unable to determine the cause of your symblepharon, they may recommend further testing, such as an eye swab or a blood test. While some of the causative conditions will resolve with therapy, others might be long-term conditions that may persist and require continuous care.
What Are the Treatment Options for Symblepharon?
Are you wondering “How to remove symblepharon?” here is your simple answer:
Latest Treatment Options (2026) focuses on:
Stopping inflammation
Preventing or removing scar tissue
Preventing symblepharon is better than treating it. Your doctors advise you the ways to prevent symblephara (plural of symblepharon) if they are aware of your predisposition to them or if you have a disease that could cause them. They manage this by treating your underlying ailment and preventing inflammation between the surfaces of your conjunctiva. Your underlying disease may be treated medically by:
Corticosteroids for inflammation
Antibiotics or antivirals for infections
Immunomodulators for autoimmune disease
Oral medications or as ocular drops may be advised. After your eye’s irritation has subsided, your doctor could apply an amniotic membrane covering to assist prevent or minimize scarring. In certain situations, they could surgically affix it to your eye, or it might be a disc that adheres like a contact lens.
You could require surgery to remove the adhesions if your doctor is unable to prevent symblepharon or is treating you after you have experienced it. The severity of symblepharon determines the type of surgery that is required. You could just require a simple operation, or you might require extensive oculoplastic surgery. Following are the techniques included:
Medical and early phase treatments
Treatment type | How it works |
Corticosteroids (drops / oral) | Reduce conjunctival |
Antibiotics / antivirals | Treat bacterial or viral |
Lubricating / preservative‑free | Protect the ocular surface and |
Immunosuppressants / | For autoimmune causes like |
Amniotic membrane transplant | Applied as a “bandage” to |
Surgical treatments for established symblepharon
Procedure | What it involves |
Symblepharon release | Cutting the adhesions between the two conjunctival layers; may include scar excision. |
Tissue graft (conjunctival/oral mucosa) | Patching denuded areas with healthy tissue to prevent re‑adhesion. |
Fornix reconstruction | Rebuilding the conjunctival fornix to restore normal eye movement and tear‑film. |
Oculoplastic reconstruction | Lid and contour repair for cosmetic and functional improvement. |
Keratoplasty (corneal transplant) | If the cornea is severely scarred or damaged. |
When Can Symblepharon Be Managed Without Surgery?
In early or mild cases, aggressive control of inflammation and protection of the ocular surface can prevent adhesions from becoming permanent. Surgery is usually reserved for fixed bands, fornix loss, or when vision or comfort is affected.
When is surgery usually needed?
Scenario | Likely management approach |
Mild or early adhesion, no functional loss | Observation + medical therapy + lubricants. |
Visible band but preserved movement | Consider early symblepharon release to prevent |
Restricted eye movement or diplopia | Symblepharon release ± grafting ± fornix |
Cosmesis or pre‑surgery (e.g., cataract/ contact | Surgery to free the fornix and improve surgical |
Blind or very painful eye | Palliative surgery to relieve discomfort and |
Does Symblepharon Come Back?
Yes, recurrence is possible, especially if:
Underlying disease is uncontrolled
Post-surgery care is inadequate
Long-term follow-up is essential.
What Study Says?
A 2024 case report found that advanced symblepharon management should focus on pain relief and quality of life, not vision recovery.
Treat the underlying cause
Address psychological factors
Accept that vision loss may be irreversible
One-Line Summary: A 2024 case report concluded that treating symblepharon requires managing the cause, supporting mental health, and prioritizing comfort since vision often cannot be restored.
Conclusion
Most of the time, a symblepharon has no symptoms. It could only be identified by your doctor during a routine eye examination. If there aren’t any signs yet, it probably won’t do any damage. Determining the cause of your symblepharon and preventing more scarring are the most crucial things to do.
Get personalized advice on managing symblepharon at Wavikar Eye Institute.
Disclaimer
This content is for informational purposes only and does not replace professional medical advice. Please consult a qualified ophthalmologist for proper diagnosis and treatment of any eye condition.










